
Preventive Care in Nursing and Midwifery Journal

Volume 15, Issue 2 (10-2025)
PCNM 2025, 15(2): 50-58 |
Back to browse issues page
Ethics code: IR.SHMU.REC.1398.025
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
ghaffari sardasht F, sadeghi M, Keramat A. Women’s satisfaction with preconception care and childbearing counseling services: a cross-sectional study. PCNM 2025; 15 (2) :50-58
URL: http://nmcjournal.zums.ac.ir/article-1-973-en.html
URL: http://nmcjournal.zums.ac.ir/article-1-973-en.html
Phd in Reproductive health, school of nursing and midwifery, medical sciences university of Neyshabur,Neyshabur,Iran , ghaffarisf3@mums.ac.ir
Keywords: Preconception care, Childbearing counseling, Reproductive health services, Quality of health care
Full-Text [PDF 739 kb]
(99 Downloads)
| Abstract (HTML) (349 Views)
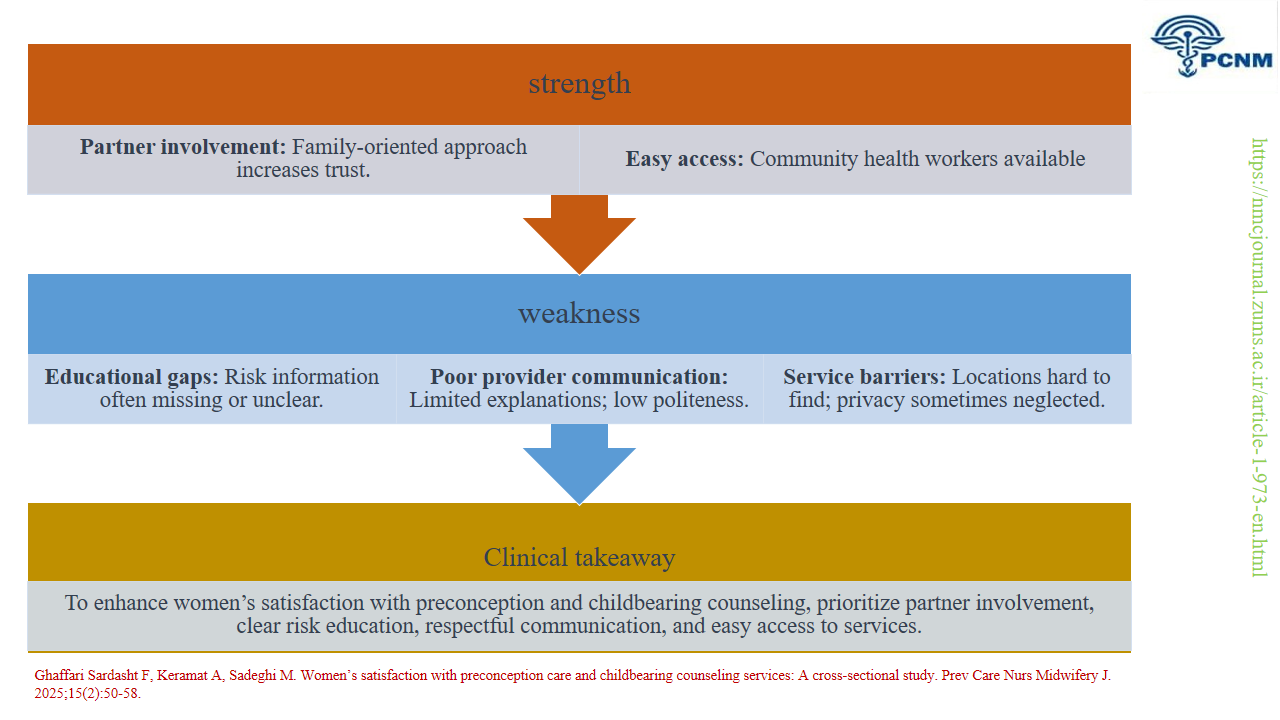
Table 1. Demographic Characteristics of Participants
(N = 319)
Table 2. Obstetric and Reproductive History of Participants (N = 319)

Full-Text: (45 Views)
Introduction
Reproductive health encompasses the biological processes, functions, and systems involved in reproduction throughout life [1]. It affirms individuals' rights to a responsible, satisfying, and safe sexual life, along with the freedom and capacity to decide if, when, and how often to have children [1]. Central to this concept is access to safe, effective, and acceptable contraceptive methods, as well as appropriate healthcare services enabling women to go safely through pregnancy and childbirth [2].
Furthermore, reproductive health acknowledges that women's needs extend beyond their reproductive years, with ongoing health issues related to the reproductive system remaining significant throughout life [3]. In Iran, the Healthy Reproductive and Childbearing Program was established to promote healthy fertility behaviors, encourage timely childbearing, and prevent infertility, thereby improving fertility rates [4].
Aligning with these objectives, the United Nations Sustainable Development Goals emphasize reducing maternal mortality and improving maternal health, all of which depend on effective reproductive health services [5]. The healthy reproductive program offers pregnancy planning and preconception counseling tailored to women's reproductive goals [6].
Ideally, both partners should be physically and mentally prepared for childbearing, with decisions informed by age and overall health status [7]. Professional organizations recommend that all women of reproductive age receive preconception care to improve pregnancy outcomes and women's health by preventing and managing risk factors that may affect pregnancy [8]. Preconception care should be integrated into primary healthcare, benefiting adolescents and young adults by promoting planned pregnancies [9,10].
Globally, significant unmet needs for family planning contribute to millions of unintended pregnancies annually [11]. Family planning services consequently play a crucial role in promoting preconception care, as planned pregnancies are associated with greater engagement with these services [12]. Counseling provides an essential opportunity to discuss the benefits of preconception care [13]. There is consequently a need for enhanced training in counseling skills for healthcare professionals to support fertility-promoting policies [14].
In recent years, Iran has implemented various initiatives to encourage higher fertility through providing reproductive health services at comprehensive health centers [15]. However, limited research exists on the quality of services in these settings. According to Donabedian's model, patient and family satisfaction are key outcome indicators reflecting care quality and effectiveness [16].
Objectives
Therefore, this study aimed to assess women's satisfaction with childbearing counseling and preconception care services provided in urban comprehensive health centers of Shahroud, Iran, and to identify key determinants influencing their satisfaction levels.
Methods
Study Design and Setting
This cross-sectional study was conducted from May to December 2022 at urban Comprehensive Health Service Centers in Shahroud, Iran. These centers provide integrated reproductive health services, including childbearing counseling and preconception care, within Iran's national primary health care network.
Study Population and Sampling
Reproductive health encompasses the biological processes, functions, and systems involved in reproduction throughout life [1]. It affirms individuals' rights to a responsible, satisfying, and safe sexual life, along with the freedom and capacity to decide if, when, and how often to have children [1]. Central to this concept is access to safe, effective, and acceptable contraceptive methods, as well as appropriate healthcare services enabling women to go safely through pregnancy and childbirth [2].
Furthermore, reproductive health acknowledges that women's needs extend beyond their reproductive years, with ongoing health issues related to the reproductive system remaining significant throughout life [3]. In Iran, the Healthy Reproductive and Childbearing Program was established to promote healthy fertility behaviors, encourage timely childbearing, and prevent infertility, thereby improving fertility rates [4].
Aligning with these objectives, the United Nations Sustainable Development Goals emphasize reducing maternal mortality and improving maternal health, all of which depend on effective reproductive health services [5]. The healthy reproductive program offers pregnancy planning and preconception counseling tailored to women's reproductive goals [6].
Ideally, both partners should be physically and mentally prepared for childbearing, with decisions informed by age and overall health status [7]. Professional organizations recommend that all women of reproductive age receive preconception care to improve pregnancy outcomes and women's health by preventing and managing risk factors that may affect pregnancy [8]. Preconception care should be integrated into primary healthcare, benefiting adolescents and young adults by promoting planned pregnancies [9,10].
Globally, significant unmet needs for family planning contribute to millions of unintended pregnancies annually [11]. Family planning services consequently play a crucial role in promoting preconception care, as planned pregnancies are associated with greater engagement with these services [12]. Counseling provides an essential opportunity to discuss the benefits of preconception care [13]. There is consequently a need for enhanced training in counseling skills for healthcare professionals to support fertility-promoting policies [14].
In recent years, Iran has implemented various initiatives to encourage higher fertility through providing reproductive health services at comprehensive health centers [15]. However, limited research exists on the quality of services in these settings. According to Donabedian's model, patient and family satisfaction are key outcome indicators reflecting care quality and effectiveness [16].
Objectives
Therefore, this study aimed to assess women's satisfaction with childbearing counseling and preconception care services provided in urban comprehensive health centers of Shahroud, Iran, and to identify key determinants influencing their satisfaction levels.
Methods
Study Design and Setting
This cross-sectional study was conducted from May to December 2022 at urban Comprehensive Health Service Centers in Shahroud, Iran. These centers provide integrated reproductive health services, including childbearing counseling and preconception care, within Iran's national primary health care network.
Study Population and Sampling
The study population comprised women of reproductive age (15-49 years) who attended the selected health centers for preconception care during the study period. The sample size was calculated based on parameters from Ghaffari et al.'s study [17], using a design effect of 1.3 to account for cluster sampling. The initial sample size of 245 was multiplied by the design effect, yielding a final sample of 319 participants.
A Multi-Stage Sampling Strategy Was Employed
A Multi-Stage Sampling Strategy Was Employed
- All 10 urban health centers in Shahroud County were included
- Proportional quotas were assigned to each center based on their registered population of reproductive-aged women
- Consecutive sampling was performed within each center until quota fulfillment
Inclusion criteria were: Iranian nationality, permanent residence in Shahroud, reproductive age (15-49 years), literacy, Persian language fluency, and physical/mental capacity to complete the questionnaire. Exclusion criteria included: healthcare employment, infertility history, current pregnancy, diagnosed psychiatric disorders, or current psychoactive medication use.
Instruments
Data were collected using a researcher-developed questionnaire measuring satisfaction with the Healthy Reproductive and Childbearing Program. The instrument contained 35 items across two domains:
Preconception care (24 items, score range: 24-120)
Childbearing counseling (11 items, score range: 11-55)
Items used a 5-point Likert scale (1 = very dissatisfied to 5 = very satisfied). Domain scores were summed for an overall satisfaction score (range: 35-175). Satisfaction levels were categorized as: strongly dissatisfied/dissatisfied (0-25%), no opinion (26-50%), satisfied (51-75%), and very satisfied (76-100%).
Content validity was established through Lawshe's method (CVR ≥ 0.56) and Waltz & Bausell's criteria (CVI ≥ 0.70) by a 12-expert panel including obstetricians, senior midwives, and public health specialists. Reliability was confirmed with Cronbach's alpha coefficients of 0.919 for pre-pregnancy care and 0.893 for fertility counseling. Confirmatory factor analysis demonstrated acceptable model fit (χ²/df = 2.42, CFI = 0.93, TLI = 0.91, RMSEA = 0.056, SRMR = 0.048), confirming construct validity.
Data Collection Procedure
Eligible participants were approached immediately after their counseling sessions. After explaining study purposes and obtaining written informed consent, questionnaires were administered in private rooms. Literate participants self-completed the survey, while those with limited literacy were interviewed. Data collection required approximately 15-20 minutes per participant. Completed questionnaires were checked for completeness before secure data transfer.
Data Analysis
Data analysis was performed using SPSS version 22. Continuous variables were described using means and standard deviations, while categorical variables were summarized with frequencies and percentages. Satisfaction scores were calculated as percentages of maximum possible scores and categorized accordingly.
Results
The participants (N=319) had a mean age of 29.20 years (SD=7.79) and a mean duration of marriage of 9.13 years (SD=6.29). Most participants were housewives (61.4%), and the most common occupation among their husbands was self-employment (39.8%) (Table 1).
Among the participants, 69.6% had been pregnant between one and five times. Of those with a pregnancy history, 86.03% had experienced at least one childbirth, and 22.9% reported a history of abortion (Table 2).
The mean satisfaction score for childbearing counseling was 29.59 )8.34( (53.8% of the maximum score). For preconception care, the mean score was 56.59 )15.67( (47.2% of the maximum). The overall satisfaction score was 86.18 )20.76( (49.2% of the maximum), indicating moderate to low satisfaction levels (Table 3).
In childbearing counseling, the item "counseling conducted with husband present" received the highest agreement (36.1% strongly agree). In contrast, "sufficient and understandable education" received the lowest agreement (0.6% strongly agree). Only 19.4% of participants agreed that risks of delayed childbearing were clearly explained (Table 4)
Instruments
Data were collected using a researcher-developed questionnaire measuring satisfaction with the Healthy Reproductive and Childbearing Program. The instrument contained 35 items across two domains:
Preconception care (24 items, score range: 24-120)
Childbearing counseling (11 items, score range: 11-55)
Items used a 5-point Likert scale (1 = very dissatisfied to 5 = very satisfied). Domain scores were summed for an overall satisfaction score (range: 35-175). Satisfaction levels were categorized as: strongly dissatisfied/dissatisfied (0-25%), no opinion (26-50%), satisfied (51-75%), and very satisfied (76-100%).
Content validity was established through Lawshe's method (CVR ≥ 0.56) and Waltz & Bausell's criteria (CVI ≥ 0.70) by a 12-expert panel including obstetricians, senior midwives, and public health specialists. Reliability was confirmed with Cronbach's alpha coefficients of 0.919 for pre-pregnancy care and 0.893 for fertility counseling. Confirmatory factor analysis demonstrated acceptable model fit (χ²/df = 2.42, CFI = 0.93, TLI = 0.91, RMSEA = 0.056, SRMR = 0.048), confirming construct validity.
Data Collection Procedure
Eligible participants were approached immediately after their counseling sessions. After explaining study purposes and obtaining written informed consent, questionnaires were administered in private rooms. Literate participants self-completed the survey, while those with limited literacy were interviewed. Data collection required approximately 15-20 minutes per participant. Completed questionnaires were checked for completeness before secure data transfer.
Data Analysis
Data analysis was performed using SPSS version 22. Continuous variables were described using means and standard deviations, while categorical variables were summarized with frequencies and percentages. Satisfaction scores were calculated as percentages of maximum possible scores and categorized accordingly.
Results
The participants (N=319) had a mean age of 29.20 years (SD=7.79) and a mean duration of marriage of 9.13 years (SD=6.29). Most participants were housewives (61.4%), and the most common occupation among their husbands was self-employment (39.8%) (Table 1).
Among the participants, 69.6% had been pregnant between one and five times. Of those with a pregnancy history, 86.03% had experienced at least one childbirth, and 22.9% reported a history of abortion (Table 2).
The mean satisfaction score for childbearing counseling was 29.59 )8.34( (53.8% of the maximum score). For preconception care, the mean score was 56.59 )15.67( (47.2% of the maximum). The overall satisfaction score was 86.18 )20.76( (49.2% of the maximum), indicating moderate to low satisfaction levels (Table 3).
In childbearing counseling, the item "counseling conducted with husband present" received the highest agreement (36.1% strongly agree). In contrast, "sufficient and understandable education" received the lowest agreement (0.6% strongly agree). Only 19.4% of participants agreed that risks of delayed childbearing were clearly explained (Table 4)
Table 1. Demographic Characteristics of Participants
(N = 319)
| Characteristic | n | % |
| Occupation | ||
| Housewife | 196 | 61.40 |
| Student | 46 | 14.40 |
| Employed | 77 | 24.10 |
| Spouse's occupation | ||
| Laborer | 75 | 23.50 |
| Employee | 76 | 23.80 |
| Farmer/Rancher | 17 | 5.30 |
| Self-employed | 127 | 39.80 |
| Student | 17 | 5.30 |
| Unemployed | 7 | 2.20 |
| Education | ||
| Illiterate | 1 | 0.30 |
| Literate (read/write) | 1 | 0.30 |
| Elementary school | 31 | 9.70 |
| Junior high school | 65 | 20.40 |
| High school/diploma | 110 | 34.50 |
| Associate's degree | 30 | 9.40 |
| Bachelor's degree | 67 | 21.00 |
| Master's degree | 14 | 4.40 |
| Spouse's education | ||
| Elementary school | 21 | 6.60 |
| Junior high school | 56 | 17.60 |
| High school/diploma | 119 | 37.30 |
| Associate's degree | 33 | 10.30 |
| Bachelor's degree | 63 | 19.70 |
| Master's degree | 23 | 7.20 |
| Doctorate | 4 | 1.30 |
| Insurance coverage | ||
| Yes | 222 | 69.60 |
| No | 97 | 30.40 |
Table 2. Obstetric and Reproductive History of Participants (N = 319)
| Characteristic | n | % |
| Underlying disease | ||
| Yes | 65 | 20.40 |
| No | 254 | 79.60 |
| Treatment for disease (n = 65) | ||
| Yes | 56 | 86.20 |
| No | 9 | 13.80 |
| History of pregnancy | ||
| Yes | 222 | 69.60 |
| No | 97 | 30.40 |
| Pregnancy complications (n = 222) | ||
| Yes | 45 | 20.30 |
| No | 177 | 79.70 |
| History of childbirth (n = 222) | ||
| Yes | 191 | 86.00 |
| No | 31 | 14.00 |
| Premature birth (n = 191) | ||
| Yes | 26 | 13.60 |
| No | 165 | 86.40 |
| Living children (n = 191) | ||
| Yes | 187 | 97.90 |
| No | 4 | 2.10 |
| History of abortion | ||
| Yes | 73 | 22.90 |
| No | 246 | 77.10 |
| Family history of congenital abnormalities | ||
| Yes | 24 | 7.50 |
| No | 295 | 92.50 |
| Contraception use | ||
| Yes | 147 | 46.10 |
| No | 172 | 53.90 |
| Prior pregnancy planning | ||
| Yes | 250 | 78.40 |
| No | 69 | 21.60 |
| Current pregnancy plans | ||
| No current plan | 144 | 45.10 |
| Currently trying to conceive | 67 | 21.00 |
| Plan in 1-3 years | 48 | 15.00 |
| Plan in 3-5 years | 43 | 13.50 |
| Trying unsuccessfully | 17 | 5.30 |
| Reason for preconception care visit | ||
| Self-referred | 125 | 39.20 |
| Health center invitation | 116 | 36.40 |
| Referred during other visit | 78 | 24.50 |
| Previous preconception care | ||
| Yes | 117 | 36.70 |
| No | 202 | 63.30 |
Table 3. Descriptive Statistics for Satisfaction Scores with Healthy Fertility Services (N = 319)
Table 4. Distribution of Responses Regarding Satisfaction with Childbearing Counseling (N = 319)
| Domain | No. of items | Minimum | Maximum | Mean | SD | Possible range |
| Childbearing counseling | 11 | 11 | 52 | 29.59 | 8.34 | 11-55 |
| Preconception care | 24 | 24 | 92 | 56.59 | 15.67 | 24-120 |
| Total satisfaction | 35 | 35 | 144 | 86.18 | 20.76 | 35-175 |
| Item | Strongly disagree | disagree | Neutral | agree | Strongly agree |
| Counseling content | |||||
| Age conditions reviewed | 22.88 | 45.45 | 16.88 | 10.99 | 3.80 |
| Health conditions reviewed | 18.50 | 37.90 | 24.80 | 16.60 | 2.20 |
| Disadvantages of delayed childbearing explained | 15.70 | 41.10 | 23.80 | 16.00 | 3.40 |
| Disadvantages of having only one child explained | 13.20 | 26.30 | 30.10 | 22.60 | 7.80 |
| Effect of age on fertility explained | 13.80 | 25.10 | 31.30 | 22.60 | 7.20 |
| Counseling process | |||||
| Counseling conducted with husband present | 7.20 | 11.90 | 13.50 | 31.30 | 36.10 |
| Freedom of choice in reproductive decisions | 24.08 | 38.56 | 22.28 | 13.49 | 1.59 |
| Sufficient and understandable education | 27.90 | 38.20 | 27.30 | 6.00 | 0.60 |
| All questions answered adequately | 17.60 | 28.20 | 35.70 | 16.00 | 2.50 |
| Use of educational tools (pamphlets, videos) | 10.31 | 10.71 | 14.41 | 35.74 | 28.83 |
| Optimal duration of education | 26.00 | 36.70 | 26.00 | 8.80 | 2.50 |
For preconception care, "ease of locating service site" received the highest disagreement (64.9% strongly disagree), while "midwife's polite behavior" received the lowest strong agreement (1.3%). Other items with low satisfaction included "short waiting time for care" (47.3% strongly disagree) and "maintained body coverage during examination" (64.9% strongly disagree) (Table 5).
No significant associations were found between satisfaction scores and age, occupation, delivery type, or parity (p>0.05). However, husband's occupation showed a significant association with satisfaction scores (F=6.692, p<0.001).
Discussion
The findings of this study indicate that women's overall satisfaction with preconception care and childbearing counseling services in Shahroud's urban health centers was below desirable levels. This is particularly evident in domains of educational adequacy, clarity of explanations, staff politeness, and accessibility of health services. These results reflect not only operational shortcomings but also deeper cultural, social, and organizational factors influencing women's perceptions of reproductive healthcare quality in Iran [18].
The higher satisfaction observed when counseling was conducted with husbands present aligns with Iran's family-oriented cultural structure, where childbearing decisions are typically made jointly [19]. This finding is consistent with previous research emphasizing that family participation enhances emotional support and psychological security for women during counseling sessions [20].
Only 19.4% of participants reported adequate explanations about risks associated with delayed childbearing, revealing significant educational gaps. Similar deficiencies in information delivery have been documented in other developing countries and are known to undermine women's trust in healthcare systems [21]. This educational shortcoming represents a critical area for improvement in service delivery.
No significant associations were found between satisfaction scores and age, occupation, delivery type, or parity (p>0.05). However, husband's occupation showed a significant association with satisfaction scores (F=6.692, p<0.001).
Discussion
The findings of this study indicate that women's overall satisfaction with preconception care and childbearing counseling services in Shahroud's urban health centers was below desirable levels. This is particularly evident in domains of educational adequacy, clarity of explanations, staff politeness, and accessibility of health services. These results reflect not only operational shortcomings but also deeper cultural, social, and organizational factors influencing women's perceptions of reproductive healthcare quality in Iran [18].
The higher satisfaction observed when counseling was conducted with husbands present aligns with Iran's family-oriented cultural structure, where childbearing decisions are typically made jointly [19]. This finding is consistent with previous research emphasizing that family participation enhances emotional support and psychological security for women during counseling sessions [20].
Only 19.4% of participants reported adequate explanations about risks associated with delayed childbearing, revealing significant educational gaps. Similar deficiencies in information delivery have been documented in other developing countries and are known to undermine women's trust in healthcare systems [21]. This educational shortcoming represents a critical area for improvement in service delivery.
| Item | Strongly disagree | disagree | Neutral | agree | Strongly agree |
| Facility and accessibility | |||||
| Easy to find a care location | 64.90 | 22.90 | 7.80 | 4.10 | 0.30 |
| Short waiting time for care | 47.30 | 22.30 | 9.10 | 19.10 | 2.20 |
| Suitable waiting space | 45.80 | 21.60 | 11.60 | 17.90 | 3.10 |
| Desirable examination room conditions | 49.50 | 27.30 | 9.10 | 11.60 | 2.50 |
| Suitable care room | 49.80 | 22.90 | 11.90 | 13.50 | 1.90 |
| Midwife-related care | 16.60 | 24.50 | 32.90 | 24.10 | 1.90 |
| Maintained body coverage during examination | 64.90 | 22.90 | 7.80 | 4.10 | 0.30 |
| Adequate guidance from a midwife | 19.70 | 23.20 | 24.50 | 26.30 | 6.30 |
| Easy to ask questions to the midwife | 47.60 | 34.50 | 10.10 | 7.20 | 0.60 |
| Confidence in the midwife's ability | 44.20 | 28.50 | 23.20 | 3.40 | 0.70 |
| Polite behavior from the midwife | 55.80 | 32.30 | 6.90 | 3.80 | 1.20 |
| Confidentiality maintained | 24.50 | 23.20 | 39.50 | 7.20 | 5.60 |
| Physician-related care | |||||
| Comfort during a physician visit | 20.10 | 21.30 | 23.80 | 23.50 | 11.30 |
| Physician's polite behavior | 34.50 | 42.60 | 16.60 | 5.00 | 1.30 |
| The physician listened carefully | 17.90 | 15.70 | 27.60 | 26.60 | 12.20 |
| Thorough examination by a physician | 14.10 | 12.60 | 28.80 | 30.40 | 14.10 |
| Explanation of required tests | 27.90 | 39.50 | 25.10 | 5.00 | 2.50 |
| Understandable explanations by the physician | 27.30 | 28.20 | 34.20 | 9.10 | 1.20 |
| Confidence in the physician's ability | 22.60 | 19.80 | 18.80 | 26.30 | 12.50 |
| Short waiting time for the physician | 18.50 | 16.30 | 26.60 | 22.30 | 16.30 |
| Opportunity to ask questions to the physician | 30.10 | 31.30 | 27.30 | 8.80 | 2.50 |
| Education | |||||
| Sufficient and understandable education | 37.90 | 30.10 | 26.00 | 5.30 | 0.70 |
| All questions answered | 18.20 | 16.90 | 43.90 | 17.90 | 3.10 |
| Use of educational tools | 9.70 | 10.30 | 11.60 | 40.80 | 27.60 |
| Optimal education duration | 31.70 | 36.40 | 24.80 | 5.00 | 2.10 |
The high dissatisfaction with service accessibility and wayfinding difficulties highlights infrastructural limitations within the healthcare facilities. These findings are consistent with research from similar settings where physical infrastructure and administrative processes significantly impact patient satisfaction [22].
The low satisfaction with staff politeness (1.3% strongly agree) suggests underlying issues related to workload, staffing shortages, and insufficient training in interpersonal communication [23]. Previous studies have demonstrated that respectful and professional interactions are crucial determinants of satisfaction with reproductive health services [24].
The current findings align with earlier evaluations of Iran's Health Transformation Plan, which noted improvements in structural aspects but persistent weaknesses in educational and counseling components [25]. This suggests that even with standardized service delivery systems, the human and relational dimensions of care require focused attention.
Based on the findings of this study, women perceived preconception counseling not merely as medical advice but as a dynamic and interactive process that guides informed reproductive decisions. Improving women’s satisfaction, therefore, calls for a shift toward a more participatory and family-oriented counseling model—one that resonates with national reproductive health policies aimed at strengthening family life and encouraging healthy childbearing. Building trust through culturally sensitive and inclusive counseling can effectively contribute to broader national goals for fertility promotion. In summary, the study revealed a significant association between the husband’s occupational status and women’s satisfaction with fertility counseling and preconception care. This relationship underscores the crucial role of socioeconomic stability and spousal support in shaping the perceived quality of reproductive health services. Accordingly, adopting a family-centered, partner-inclusive approach in program planning and service delivery is essential for enhancing women’s satisfaction and optimizing care outcomes.
This study has several limitations. The sample was restricted to women attending public urban health centers in Shahroud, potentially limiting generalizability. Self-reported data may be subject to recall and social desirability biases. Additionally, some cultural and interpersonal dimensions of satisfaction might not have been fully captured by the survey instruments.
Conclusion
The moderate to low satisfaction levels identified in this study primarily stem from insufficient education, weak provider-client communication, and structural barriers. While services provided by community health workers were viewed more favorably, significant gaps remain in both educational content and care processes. Quality improvement initiatives should focus on enhancing staff communication skills, developing culturally appropriate educational materials, and improving physical infrastructure. Future research should employ qualitative methods to better understand the underlying barriers to satisfaction and evaluate targeted interventions to enhance both structural and process aspects of reproductive health services.
Ethical Considerations
This study received approval from the Ethics Committee of Shahroud University of Medical Sciences (Code: IR.SHMU.REC.1398.025). Written informed consent was obtained from all participants before their involvement in the study. Participants were assured of the confidentiality of their information, and the principle of anonymity was maintained throughout the research process.
Acknowledgments
This research was conducted as part of the project "Evaluation of the Existing Preconception Care Program in Iran, Its Modification, and Pilot Implementation" (Project Code: 9815), approved by Shahroud University of Medical Sciences under ethics code IR.SHMU.REC.1398.025. The authors extend their sincere gratitude to all the women who participated in this study for their valuable contributions.
Conflict of Interest
The authors declare that there are no conflicts of interest associated with the publication of this research.
Funding
This study did not receive any financial support from public, commercial, or not-for-profit funding agencies.
Authors' Contributions
All authors made substantial contributions to this study. FGh was responsible for data acquisition, manuscript drafting, and revision. MS contributed to data collection. AK was responsible for the accuracy of implementation and interpretation of the study. All authors reviewed and approved the final version of the manuscript.
Artificial Intelligence Utilization
During manuscript preparation, minor assistance from artificial intelligence (AI) tools was utilized to enhance English phrasing and improve the clarity of scientific writing. All analytical decisions and final editing were performed by the authors. The use of AI complied with ethical standards of academic publishing and did not replace author responsibility.
Data Availability Statement
The dataset supporting the findings of this study is not publicly available due to privacy regulations protecting participant confidentiality. However, the data may be made available from the corresponding author upon reasonable request. For transparency purposes, de-identified SPSS data files used in exploratory and confirmatory factor analyses are securely stored and can be shared for academic verification.
The low satisfaction with staff politeness (1.3% strongly agree) suggests underlying issues related to workload, staffing shortages, and insufficient training in interpersonal communication [23]. Previous studies have demonstrated that respectful and professional interactions are crucial determinants of satisfaction with reproductive health services [24].
The current findings align with earlier evaluations of Iran's Health Transformation Plan, which noted improvements in structural aspects but persistent weaknesses in educational and counseling components [25]. This suggests that even with standardized service delivery systems, the human and relational dimensions of care require focused attention.
Based on the findings of this study, women perceived preconception counseling not merely as medical advice but as a dynamic and interactive process that guides informed reproductive decisions. Improving women’s satisfaction, therefore, calls for a shift toward a more participatory and family-oriented counseling model—one that resonates with national reproductive health policies aimed at strengthening family life and encouraging healthy childbearing. Building trust through culturally sensitive and inclusive counseling can effectively contribute to broader national goals for fertility promotion. In summary, the study revealed a significant association between the husband’s occupational status and women’s satisfaction with fertility counseling and preconception care. This relationship underscores the crucial role of socioeconomic stability and spousal support in shaping the perceived quality of reproductive health services. Accordingly, adopting a family-centered, partner-inclusive approach in program planning and service delivery is essential for enhancing women’s satisfaction and optimizing care outcomes.
This study has several limitations. The sample was restricted to women attending public urban health centers in Shahroud, potentially limiting generalizability. Self-reported data may be subject to recall and social desirability biases. Additionally, some cultural and interpersonal dimensions of satisfaction might not have been fully captured by the survey instruments.
Conclusion
The moderate to low satisfaction levels identified in this study primarily stem from insufficient education, weak provider-client communication, and structural barriers. While services provided by community health workers were viewed more favorably, significant gaps remain in both educational content and care processes. Quality improvement initiatives should focus on enhancing staff communication skills, developing culturally appropriate educational materials, and improving physical infrastructure. Future research should employ qualitative methods to better understand the underlying barriers to satisfaction and evaluate targeted interventions to enhance both structural and process aspects of reproductive health services.
Ethical Considerations
This study received approval from the Ethics Committee of Shahroud University of Medical Sciences (Code: IR.SHMU.REC.1398.025). Written informed consent was obtained from all participants before their involvement in the study. Participants were assured of the confidentiality of their information, and the principle of anonymity was maintained throughout the research process.
Acknowledgments
This research was conducted as part of the project "Evaluation of the Existing Preconception Care Program in Iran, Its Modification, and Pilot Implementation" (Project Code: 9815), approved by Shahroud University of Medical Sciences under ethics code IR.SHMU.REC.1398.025. The authors extend their sincere gratitude to all the women who participated in this study for their valuable contributions.
Conflict of Interest
The authors declare that there are no conflicts of interest associated with the publication of this research.
Funding
This study did not receive any financial support from public, commercial, or not-for-profit funding agencies.
Authors' Contributions
All authors made substantial contributions to this study. FGh was responsible for data acquisition, manuscript drafting, and revision. MS contributed to data collection. AK was responsible for the accuracy of implementation and interpretation of the study. All authors reviewed and approved the final version of the manuscript.
Artificial Intelligence Utilization
During manuscript preparation, minor assistance from artificial intelligence (AI) tools was utilized to enhance English phrasing and improve the clarity of scientific writing. All analytical decisions and final editing were performed by the authors. The use of AI complied with ethical standards of academic publishing and did not replace author responsibility.
Data Availability Statement
The dataset supporting the findings of this study is not publicly available due to privacy regulations protecting participant confidentiality. However, the data may be made available from the corresponding author upon reasonable request. For transparency purposes, de-identified SPSS data files used in exploratory and confirmatory factor analyses are securely stored and can be shared for academic verification.
Type of Study: Orginal research |
Subject:
Midwifery
Received: 2025/07/12 | Accepted: 2025/10/2 | Published: 2025/10/2
Received: 2025/07/12 | Accepted: 2025/10/2 | Published: 2025/10/2
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |



