Preventive Care in Nursing and Midwifery Journal

Volume 15, Issue 2 (10-2025)
PCNM 2025, 15(2): 23-31 |
Back to browse issues page
Ethics code: IR.KAUMS.NUHEPM.REC.1398.037
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Afshar M, Mazhariazad F, Taghadosi M. The correlation between burnout and quality of caring behavior among nurses: A cross-sectional study. PCNM 2025; 15 (2) :23-31
URL: http://nmcjournal.zums.ac.ir/article-1-984-en.html
URL: http://nmcjournal.zums.ac.ir/article-1-984-en.html
The correlation between burnout and quality of caring behavior among nurses: A cross-sectional study
Department of Nursing BA.C, Islamic Azad University, Bandar Abbas, Iran. , f.mazhariazad@iau.ac.ir
Abstract: (156 Views)
Background: Occupational stress and burnout are significant issues in healthcare professions that can impact caring behaviors.
Objectives: The study aimed to investigate the correlation between burnout and the quality of caring behaviors among nurses working in hospitals affiliated with Kashan University of Medical Sciences.
Methods: This cross-sectional analytical study included 212 nurses from hospitals affiliated with Kashan University of Medical Sciences. Data were collected using demographic questionnaires, the Caring Behaviors Inventory, and the Maslach Burnout Inventory, and analyzed with SPSS version 26 using descriptive statistics, linear regression, and Pearson correlation.
Results: This study of 212 nurses found a favorable care quality score (M=209.96, SD=27.13). Burnout levels were M=46.24 (SD=19.20) for frequency and M=53.58 (SD=21.19) for intensity. Significant negative correlations emerged between both burnout dimensions and care quality (frequency: r=-0.327; intensity: r=-0.296, both p<.001). While personal accomplishment and depersonalization correlated with all care components (p<.01), emotional exhaustion showed no significant correlations (p>.05).
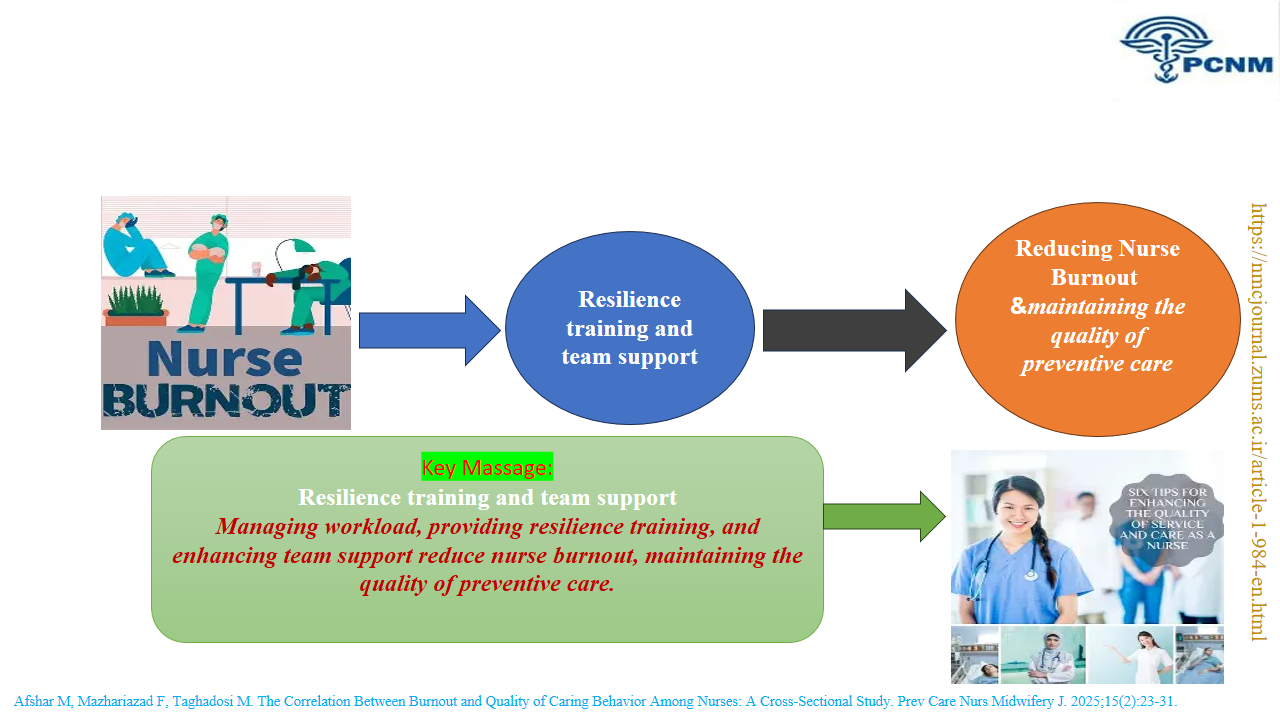
Conclusion: The study emphasizes that burnout negatively affects nurses’ ability to provide empathetic, high-quality care. Organizational measures like workload management, resilience training, and team support can reduce burnout and enhance care quality in high-stress settings.
Objectives: The study aimed to investigate the correlation between burnout and the quality of caring behaviors among nurses working in hospitals affiliated with Kashan University of Medical Sciences.
Methods: This cross-sectional analytical study included 212 nurses from hospitals affiliated with Kashan University of Medical Sciences. Data were collected using demographic questionnaires, the Caring Behaviors Inventory, and the Maslach Burnout Inventory, and analyzed with SPSS version 26 using descriptive statistics, linear regression, and Pearson correlation.
Results: This study of 212 nurses found a favorable care quality score (M=209.96, SD=27.13). Burnout levels were M=46.24 (SD=19.20) for frequency and M=53.58 (SD=21.19) for intensity. Significant negative correlations emerged between both burnout dimensions and care quality (frequency: r=-0.327; intensity: r=-0.296, both p<.001). While personal accomplishment and depersonalization correlated with all care components (p<.01), emotional exhaustion showed no significant correlations (p>.05).
Conclusion: The study emphasizes that burnout negatively affects nurses’ ability to provide empathetic, high-quality care. Organizational measures like workload management, resilience training, and team support can reduce burnout and enhance care quality in high-stress settings.
Type of Study: Orginal research |
Subject:
Nursing
Received: 2025/09/10 | Accepted: 2025/10/2 | Published: 2025/10/2
Received: 2025/09/10 | Accepted: 2025/10/2 | Published: 2025/10/2
References
1. Maslach C, Jackson SE. The Measurement of Experienced Burnout. Journal of Organizational Behavior. 1981;2(2):99-113. [https://doi.org/10.1002/job.4030020205]
2. Chung H-C, Chen Y-C, Chang S-C, Hsu W-L, Hsieh T-C. Development and Validation of Nurses’ Well-Being and Caring Nurse–Patient Interaction Model: A Psychometric Study. International Journal of Environmental Research and Public Health. 2021;18(15):7750. [https://doi.org/10.3390/ijerph18157750]
3. Zhang X, Wu Y. Roles and Contributions of Companions in Healthcare Professional-Older Patient Interaction: A Systematic Review. Patient Education and Counseling. 2025;130:108455. [https://doi.org/10.1016/j.pec.2024.108455]
4. Khatatbeh H, Pakai A, Al‐Dwaikat T, Onchonga D, Amer F, Prémusz V, et al. Nurses’ Burnout and Quality of Life: A Systematic Review and Critical Analysis of Measures Used. Nursing Open. 2022;9(3):1564-74. [https://doi.org/10.1002/nop2.936]
5. Dutra CKdR, Guirardello EdB. Nurse Work Environment and Its Impact on Reasons for Missed Care, Safety Climate, and Job Satisfaction: A Cross‐Sectional Study. Journal of Advanced Nursing. 2021;77(5):2398-406. [https://doi.org/10.1111/jan.14764]
6. Vermeir P, Blot S, Degroote S, Vandijck D, Mariman A, Vanacker T, et al. Communication Satisfaction and Job Satisfaction Among Critical Care Nurses and Their Impact on Burnout and Intention to Leave: A Questionnaire Study. Intensive and Critical Care Nursing. 2018;48:21-7. [https://doi.org/10.1016/j.iccn.2018.07.001]
7. Efıl S, Turen S, Ayvaz MY, Bulbul E, Yenı T. Burnout Levels and Care Behaviours in Intensive Care Nurses: A Cross-Sectional, Multicentre Study. Intensive and Critical Care Nursing. 2022;71:103246. [https://doi.org/10.1016/j.iccn.2022.103246]
8. Mazhariazad F, Adib HM. Concept Analysis of “Role Strain” According to Walker and Avant’s Approach. Iranian Journal of Nursing Research. 2021;16(3):29-38. [https://sid.ir/paper/984403/en]
9. Bruyneel A, Smith P, Tack J, Pirson M. Prevalence of Burnout Risk and Factors Associated With Burnout Risk Among ICU Nurses During the COVID-19 Outbreak in French Speaking Belgium. Intensive and Critical Care Nursing. 2021;65:103059. [https://doi.org/10.1016/j.iccn.2021.103059]
10. Mohammed Alhussin E, Mohamed SA, Hassan AA, Al-Qudimat AR, Doaib AM, al jonidy RM, et al. Patients’ Satisfaction With the Quality of Nursing Care: A Cross-Section Study. International Journal of Africa Nursing Sciences. 2024;20:100690. [https://doi.org/10.1016/j.ijans.2024.100690]
11. Dehghani Y, Asghari F, Saeidpour F, Joukar E. Prediction of Occupational Burnout Based on Job Satisfaction, Personality Traits and Mental Health. Iranian Journal of Nursing Research. 2017;12(5):61-70. [http://ijnr.ir/article-1-1833-en.html]
12. Khandan M, Rostami M. Investigating the Correlation Between Job Burnout and Ethical Decision Making Among Nurses Working in Intensive Care Units. Journal of Health and Care. 2024;25(3):234-44. [http://doi.org/10.61186/jhc.25.3.234]
13. Thomas D, Newcomb P, Fusco P. Perception of Caring Among Patients and Nurses. Journal of Patient Experience. 2019;6(3):194-200. [https://doi.org/10.1177/2374373518795713]
14. Azimilolaty H, Rezaei S, Khorram M, Mousavinasab N, Heidari T. Correlation Between the Quality of Nursing Care and Burnout of Nurses in the Teaching Hospitals Affiliated to Mazandaran University of Medical Sciences, Iran. Iran Journal of Nursing. 2021;33(128):54-66. [http://ijn.iums.ac.ir/article-1-3339-en.html]
15. Aghabarary M, Dehghan Nayeri N, Varvani Farahani A. Perception of Futile Care: A Qualitative Study. Hayat. 2019;24(4):381-404. [http://hayat.tums.ac.ir/article-1-2811-en.html]
16. Alikari V, Gerogianni G, Fradelos EC, Kelesi M, Kaba E, Zyga S. Perceptions of Caring Behaviors Among Patients and Nurses. International Journal of Environmental Research and Public Health. 2022;20(1):396. [https://doi.org/10.3390/ijerph20010396]
17. Jaradat Y, Qtait M. Occupational Stress and Associated Risk Factors Among Nurses in Hebron Hospitals: A Cross-Sectional Study From the West Bank, Palestine. SAGE Open Nursing. 2025;11:1-8. [https://doi.org/10.1177/23779608251374155]
18. Woo T, Ho R, Tang A, Tam W. Global Prevalence of Burnout Symptoms Among Nurses: A Systematic Review and Meta-Analysis. Journal of Psychiatric Research. 2020;123:9-20. [https://doi.org/10.1016/j.jpsychires.2019.12.015]
19. Wolf ZR, Colahan M, Costello A. Relationship Between Nurse Caring and Patient Satisfaction. Medsurg Nursing. 1998;7(2):99-105. [https://www.proquest.com/docview/230513410]
20. Hajinezhad ME, Azodi P, Rafii F, Ramezanian N, Tarighat M. Perspectives of Patients and Nurses on Caring Behaviors of Nurses. Hayat. 2012;17(4):36-45. [http://hayat.tums.ac.ir/article-1-36-en.html]
21. Askari R, Abarghouei HF, Heidarijamebozorgi M, Keyvanlo Z, Kargar M. Job Burnout Among Nurses in Iran: A Systematic Review and Meta-Analysis. Nursing and Midwifery Studies. 2021;10(2):65-72. [https://doi.org/10.4103/nms.nms_48_20]
22. Tesema TM, Golja EA, Atomsa L, Berisa YM. Perception of Caring Behaviors and Associated Factors Among Nurses Working in Public Hospitals of East Wollega Zone, Ethiopia, 2023. Mixed Method Study. Frontiers in Public Health. 2025;13:1513819. [https://doi.org/10.3389/fpubh.2025.1513819]
23. Clark RR, Lake E. Burnout, Job Dissatisfaction and Missed Care Among Maternity Nurses. Journal of Nursing Management. 2020;28(8):2001-6. [https://doi.org/10.1111/jonm.13037]
24. White EM, Aiken LH, McHugh MD. Registered Nurse Burnout, Job Dissatisfaction, and Missed Care in Nursing Homes. Journal of the American Geriatrics Society. 2019;67(10):2065-71. [https://doi.org/10.1111/jgs.16051]
25. Begjani J, Jafari M, Khajezadeh A, Rajabi MM. The Relationship Between Job Burnout and Missed Nursing Care in Nurses From the Selected Hospitals in Tehran, Iran. Iran Journal of Nursing. 2024;37(147):78-89. [http://doi.org/10.32598/ijn.37.147.3348.9]
26. Sohrabi Y, Yarmohammadi H, Pouya AB, Arefi MF, Hassanipour S, Poursadeqiyan M. Prevalence of Job Burnout in Iranian Nurses: A Systematic Review and Meta-Analysis. Work. 2022;73(3):937-43. [https://doi.org/10.3233/WOR-210283]
27. Vahedian-Azimi A, Hajiesmaeili M, Kangasniemi M, Fornés-Vives J, Hunsucker RL, Rahimibashar F, et al. Effects of Stress on Critical Care Nurses: A National Cross-Sectional Study. Journal of Intensive Care Medicine. 2019;34(4):311-22. [https://doi.org/10.1177/0885066617696853]
28. Heidari T, Azimilolaty H, Khorram M, Rezaei S, Mousavinasab S-N, Nikbakht R. Association Between Moral Intelligence, Burnout and Quality of Nursing Care. Clinical Ethics. 2022;17(4):334-45. [https://doi.org/10.1177/14777509211040168]
29. Nantsupawat A, Wichaikhum OA, Abhicharttibutra K, Sadarangani T, Poghosyan L. The Relationship Between Nurse Burnout, Missed Nursing Care, and Care Quality Following COVID-19 Pandemic. Journal of Clinical Nursing. 2023;32(15-16):5076-83. [https://doi.org/10.1111/jocn.16761]
30. Chirico F, Afolabi AA, Ilesanmi OS, Nucera G, Ferrari G, Sacco A, et al. Prevalence, Risk Factors and Prevention of Burnout Syndrome Among Healthcare Workers: An Umbrella Review of Systematic Reviews and Meta-Analyses. Journal of Health and Social Sciences. 2021;6(4):465-91. [https://doi.org/10.19204/2021/prvl3]
31. Belay AS, Guangul MM, Asmare WN, Bogale SK, Manaye GA. Prevalence and Associated Factors of Burnout Syndrome Among Nurses in Public Hospitals, South West Ethiopia. Ethiopian Journal of Health Sciences. 2021;31(3):543-52. [https://doi.org/10.4314/ejhs.v31i3.11]
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |